Obesity is defined with the body mass index (BMI)
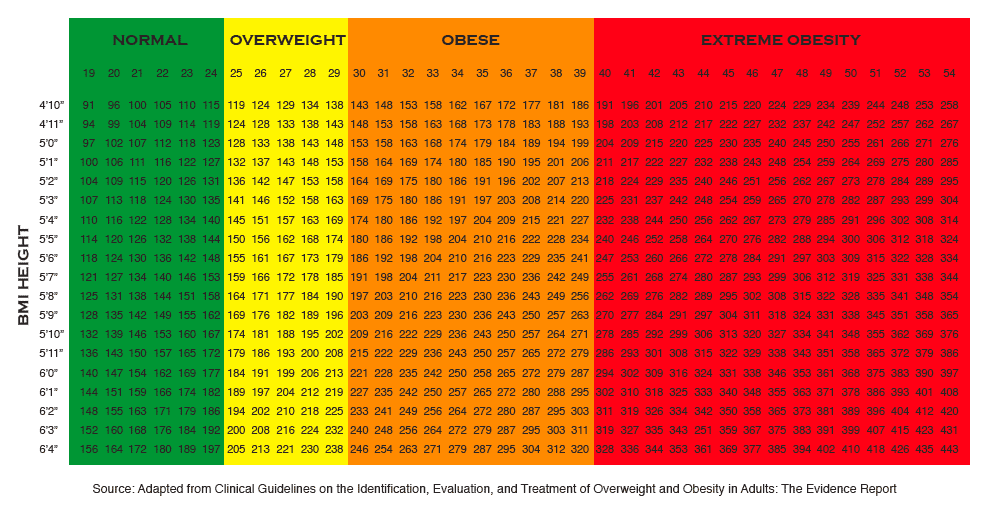
Body Mass Index (BMI) is a relationship between weight and height that is associated with body fat and health risk. Weight is converted to kilograms; height is converted to meters and then squared. Thus, BMI = kg/m2.
- BMI over 30 is obese
- BMI between 25 - 29.9 is overweight.
- BMI between 18.5 – 24.9 is healthy.
- BMI 18.4 or below is underweight
Advantages of the BMI
Disadvantages of the BMI
Obesity increases the risk of developing physical conditions including:
Obesity increases the risk of mental conditions including: Negative self-image (Holm et al, 2001)
Epidemiology: Where and among whom is obesity a problem?
According to the Behavioral Risk Factor Surveillance System
(Mokdad et al., 2001) study of 184,450 adults in the U.S. in 2000, regarding the prevalence of obesity:
Obesity % by Gender
| Male | 20.2% |
| Female | 19.4% |
Obesity % by Age
| age 18-29 | 13.5% |
| age 30-39 | 20.2% |
| age 40-49 | 22.9% |
| age 50-59 | 25.6% |
| age 60-69 | 22.9% |
| age 70+ | 15.5% |
| Less than High School | 26.1% |
| High School grad | 21.7% |
| Some College | 19.5% |
| College degree+ | 15.2% |
| Inactive | 27.0% |
| Irregularly active | 28.2% |
| Regular, not intense | 30.5% |
| Regular, intense | 14.3% |
| less than 1 | 4.0% |
| 1 to <3 | 33.1% |
| Intake 3 to <5 | 38.5% |
| >=5 | 24.4% |
Weight Control Practices
| People trying to lose wt. | 38.5% |
| Trying to maintain wt | 35.9% |
| Neither | 25.6% |
Neural Mechanisms Associated with Obesity
The hypothalamus controls energy homeostasis and the motivation to eat, that is, it contains axons and synapses of neurons that control feeding. The lateral hypothalamus is associated with hunger and the medial hypothalamus is associated with satiety. Lateral hypothalamus (LH) cells are inhibited by increases of norepinephrine and disinhibited by norepinephrine depletion.
Norepinephrine or epinephrine and dopamine can act in the lateral hypothalamus (LH) to curb feeding. However, dopamine agonists help restore reactivity to food and excess dopamine in parts of the striatum or accumbens may be a source of obesity. Thus, DA seems to potentiate feeding and reward in the accumbens and suppress feeding in the LH.
Serotonin either potentiates the paraventricular nucleus medial hypothalamus (PVN-MH) satiety system or inhibits the LH feeding system.
Appetite for specific macronutrients is controlled by specific neurotransmitters. Serotonin affects diet choice and is itself affected by the diet under certain circumstances.
Etiology: Models that theorize on the causes for obesity.
Caused by energy intake persistently exceeding metabolic energy expenditure- eating too much, exercising too little, or a combination of both.
Once attributed mainly to lack of will power, obesity is now understood to result from a complex interaction of genetic, developmental, metabolic, behavioral and environmental factors.
80% of obese patients are FH+ for obesity. Learned dietary habits may account for some obesity but twin studies and animal breeding studies indicate genetics is also a risk factor for obesity.
Developmentally, the number of fat cells is established early in life and not very susceptible to change. Overweight children establish more adipocytes and maintain them into adulthood.
Hunger is the metabolic signal to eat. Satiety is the feeling that results from hunger being satisfied. Most people are predisposed to a preference for higher fat foods, which are slower to produce satiety than low fat foods.
The olfactory system plays a role in hunger and satiety.
Appetite, the desire to eat, can be increased by psychological factors like thoughts or feelings. Binge eating can be a reaction to stress.
Obese people are more susceptible to external stimuli to eating such as food cues in the environment and they are less responsive to internal hunger. Some obese people are unable to distinguish hunger from other sources of dysphoria.
A decrease in the amount of daily activity related to work, transportation and personal chores is believed to contribute to the high percentage of overweight and obesity today.
Recommendations for Treatment of Obesity
Dietary Therapy
Dietary therapy involves instruction on how to adjust a diet to reduce the number of calories eaten. Strategies of dietary therapy include teaching about calorie content of different foods, food composition (fats, carbohydrates, and proteins), reading nutrition labels, types of foods to buy, and how to prepare foods.Physical Activity
Moderate physical activity, progressing to 30 minutes or more on most or preferably all days of the week is recommended for weight loss.Behavior Therapy
Behavior therapy involves changing diet and physical activity patterns and habits to new behaviors that promote weight loss. Behavioral therapy strategies for weight loss and maintenance include:
Four common behaviors of successful weight losers
(Bren, 2002)(study of 3,000 Americans that lost an average of 60 lbs and kept it off 6+ years)
- Low-fat, high-carbohydrate diet (24% of calories from fat)
- Weight themselves frequently
- Very physically active
- Eat breakfast every day
Drug Therapy
Drug therapy is recommended as a treatment option for persons with:
- A BMI > 30 with no obesity-related conditions
- A BMI of > 27 with two or more obesity-related conditions
Drug therapy may be used for weight loss and weight maintenance.
Three weight loss drugs, approved by the US Food and Drug Administration (FDA) for treating obesity, are orlistat, phentermine, and sibutramine. Orlistat (Xenical) is a lipase inhibitor that works by blocking about 30% of dietary fat from being absorbed. It is the most recently approved weight loss drug Phentermine is a cerebral stimulant that suppresses the appetite by increasing norepinephrine levels. It has been available for many years. The use of phentermine alone has not been associated with the adverse health effects of the fenfluramine-phentermine (fen-phen) combination. Tolerance to amphetamines is common. Sibutramine (Meridia) is an antidepressant that suppresses appetite by inhibiting reuptake of serotonin, norepinephrine and dopamine. It is approved for long-term use. Although prolonged use of serotonergic agonists for depression has been associated with weight gain.
Surgery
Obesity surgery is recommended as a treatment option for persons with obesity that have a BMI > 40 or a BMI of 35 to 39.9 with serious medical conditions. Obesity surgery is used to modify the stomach and or intestines to reduce the amount of food that can be eaten.
References:
Bren, L. (2002). Losing weight: more than counting calories. FDA Consumer 36(1) 18-26.
Holm, K., Li, S., Spector, N., Hicks, F., Carlson, E., & Lanuza, D. (2001). Obesity in adults and children: a call for action. Journal of Advanced Nursing.36(2). 266-269. Kaplan, H.I. & Sadock, B.J. (1998). Synopsis of psychiatry. 8th Ed. Baltimore, M.D., Williams & Wilkins. Mokdad, A., Bowman, B.A., Ford, E.S., Vinicor, F., Marks, J.S., & Koplan, J.P. (2001) The continueing epidemics of obesity and diabetes in the United States. Journal of the American Medical Association. 286(10) 1195-1200. Stunkard, A.J., & Wadden, T.A. (1993). Obesity theory and therapy. New York, NY: Raven Press, Ltd.